What's the difference between Digital Spirometers & Incentive Spirometers? | CMI Health

With all of the medical devices out on the market today, it can be hard to keep up with the latest innovations and figure out which products are best for you. If you’ve been feeling confused or overwhelmed about the latest and greatest medical devices, look no further! At CMI Health, we want to give our customers the most accurate information possible to make sense of what best suits their needs. Today, we will be discussing Spirometry and the key differences between the most popular spirometers on the market.
So, what is Spirometry exactly?
The American Lung Association defines Spirometry as “the most common type of pulmonary function or breathing test. This test measures how much air you can breathe in and out of your lungs, as well as how easily and fast you can blow the air out of your lungs” (AMA, 2022). Often, it is used to diagnose chronic respiratory disease or to check lung function before and after surgery. If one is already diagnosed with an illness like Asthma or COPD, Spirometry can be a useful tool to determine if lung health is improving or worsening.
The functions a Spirometer measure can be expressed as Force Vital Capacity (FVC) and Forced Expiratory Volume in 1 second (FEV1).
FVC - This is the largest amount of air that you can forcefully exhale after breathing in as deeply as you can. A lower-than-normal FVC reading indicates restricted breathing (Mayo Clinic, 2017).
FEV1 – This is how much air you can force from your lungs in one second. This reading helps your doctor assess the severity of your breathing problems. Lower FEV-1 readings indicate more significant obstruction (Mayo Clinic, 2017).
Over a prolonged period, spirometry can help track the progression of chronic respiratory illnesses and enable doctors to pinpoint the best course of action for their patients. The Spirometer you use to get these measurements may differ depending on whether you are at the doctor’s office or at home and what kind of data you want. Even so, the device functions will largely remain the same. There are mainly two different types of spirometers; Incentive Spirometers and Digital Spirometers. While they are both very useful, there are some key differences between the two devices.
Digital Spirometers

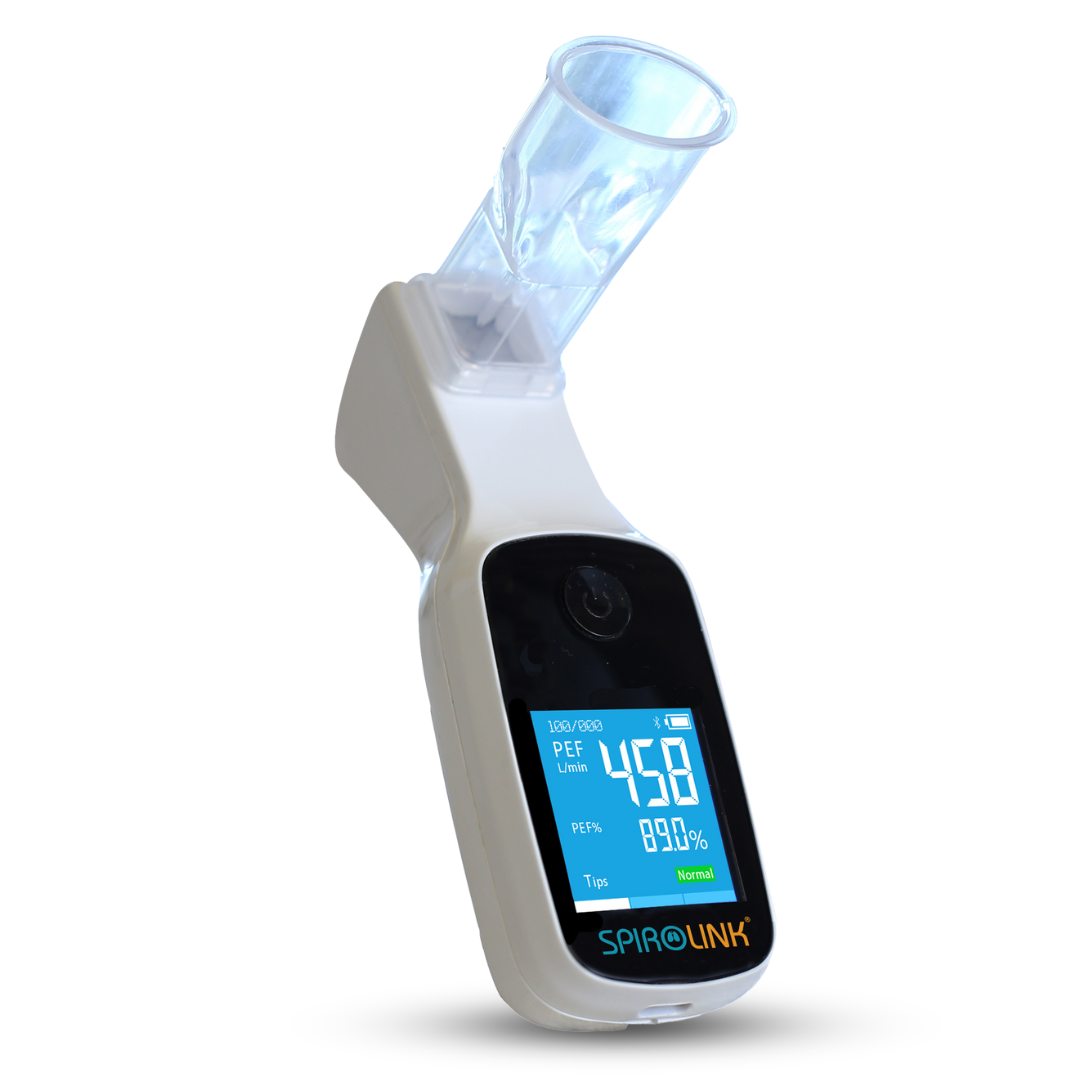
Digital Spirometers can detect significant lung obstruction and weakened breathing capabilities, which can be indicators of serious potential problems over time. Digital Spirometers are designed to create the most convenient and user-friendly experience possible. They can generate health data reports that can be sent to the user’s phone via Bluetooth, or even directly to a physician. Unlike an Incentive Spirometer, these peak flow meters measure exhaled air from the lungs through an internal turbine system. Digital Spirometers measure Forced Expiratory Volume 1 (FEV1) in the first second you inhale, Forced Vital Capacity (FVC), and Peak Expiratory Flow (PEF) (Mayo Clinic, 2017).
Digital Spirometers make the most sense for convenient, at-home use as they are often rechargeable and meticulously keep track of your lung health data, like our SpiroLink® device. They are ideal for people with chronic lung health problems, like Asthma or COPD, and for those that have careers, like athletes or musicians, where lung capacity plays a crucial role. While they differ in quality and features, we recommend looking for one that has an on-screen display and disposable filters. Sometimes, the internal turbine system can be more subject to debris and damage, which can shorten the lifespan of a Digital Spirometer. With the desire to create a long-lasting and accurate Spirometer, our SpiroLink® utilizes a pressure sensor, which can hold up against debris, dust, and mucus.
Incentive Spirometers

Incentive Spirometers, while similar, have some key differences from Digital Spirometers. They are much simpler devices that are designed to specifically improve lung capacity instead of tracking health changes over time. They are extremely helpful for promoting lung activity and expansion, preventing fluid buildup, and with deep breathing or coughing exercises (NLM, 2022). They are ideal for individuals that have recently undergone an illness or major surgery and need help with lung health recovery, whether that be in a hospital or at-home health monitoring setting.
Incentive Spirometers operate using a simple piston system. Essentially, when the user breathes in, pistons on the inside of the tube will rise, actively measuring the amount of air taken in by the lungs (Healthline, 2020). Inhaled air is the only measurement an incentive spirometer can provide, which differs from the exhaled air measurement a Digital Spirometer takes. The purpose of using an incentive spirometer is to promote lung activity and prevent fluid from building up, hindering pneumonia and other serious conditions from developing. Click here for how to properly read measurements from a Spirometer.
There are a lot of factors that can contribute to one’s decision about what the best type of Spirometer is for their specific needs. Things like device efficacy, lifespan, and types of measurements taken are all important factors to consider when purchasing a Spirometer. Click here for a more comprehensive guide to the different types of Spirometers. Follow CMI Health to stay up to date with the latest industry innovations and medical device information to take the guesswork out of purchasing important healthcare devices.
Still have questions? Feel free to contact us at info@cmihealth.com or call us at 888-985-1125 (ext. 1).























Leave a comment